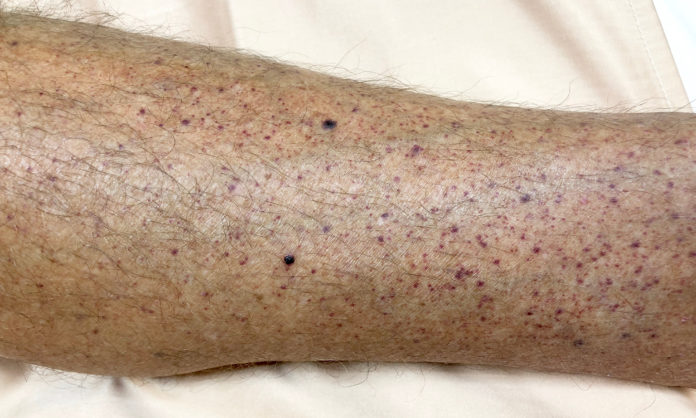
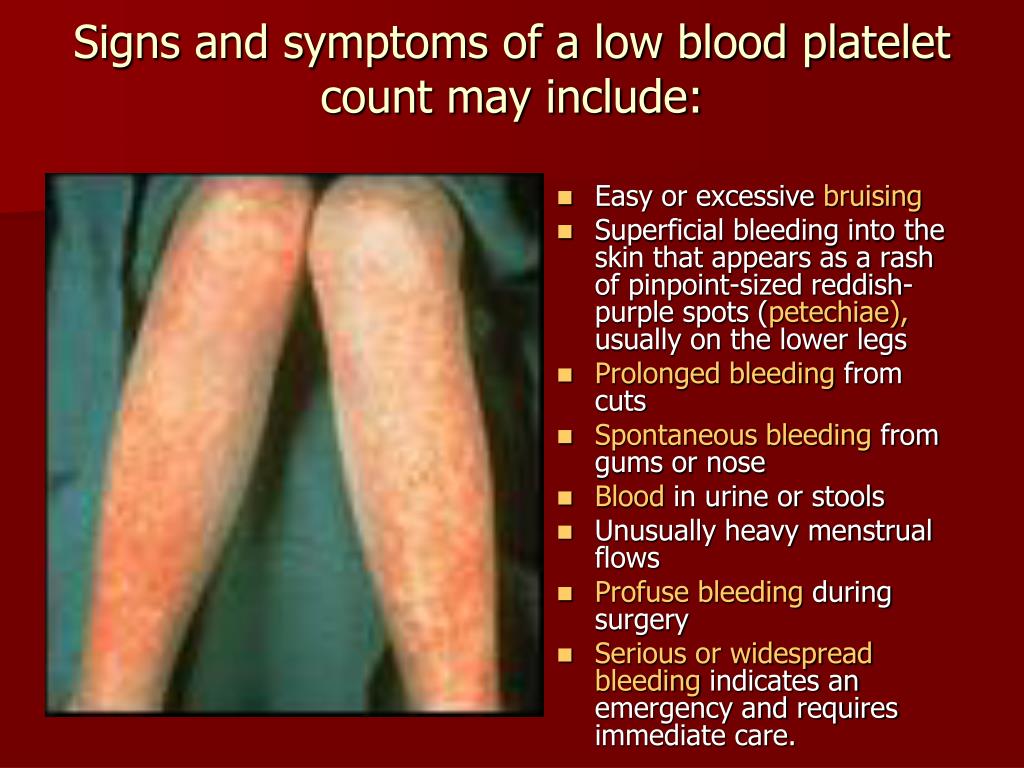
1 these figures far exceed the 3% threshold set by the national institute for health and care excellence (nice) for investigating possible cancer in the uk.Many blood cancer patients have low platelet counts because their bodies are unable to produce enough platelets.
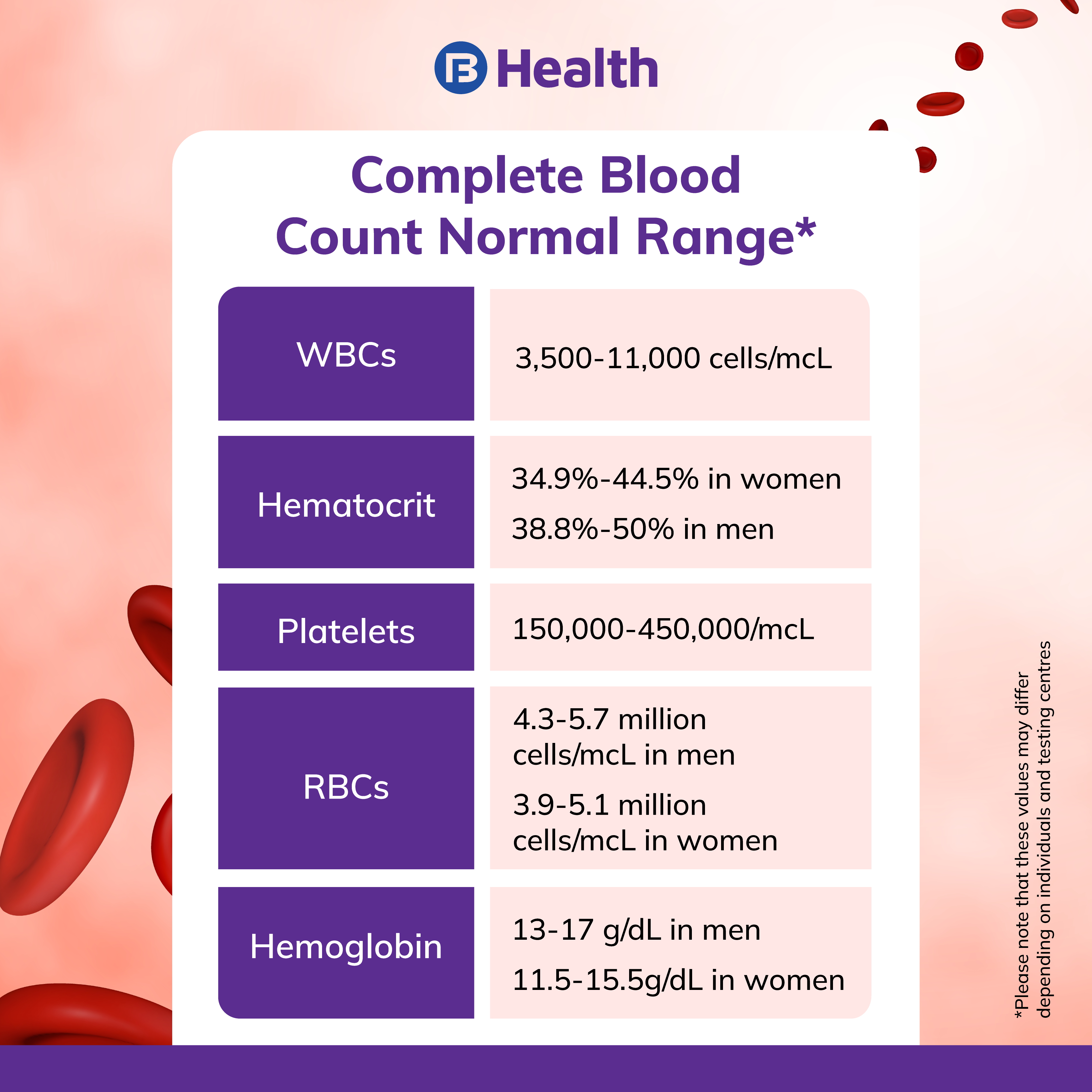
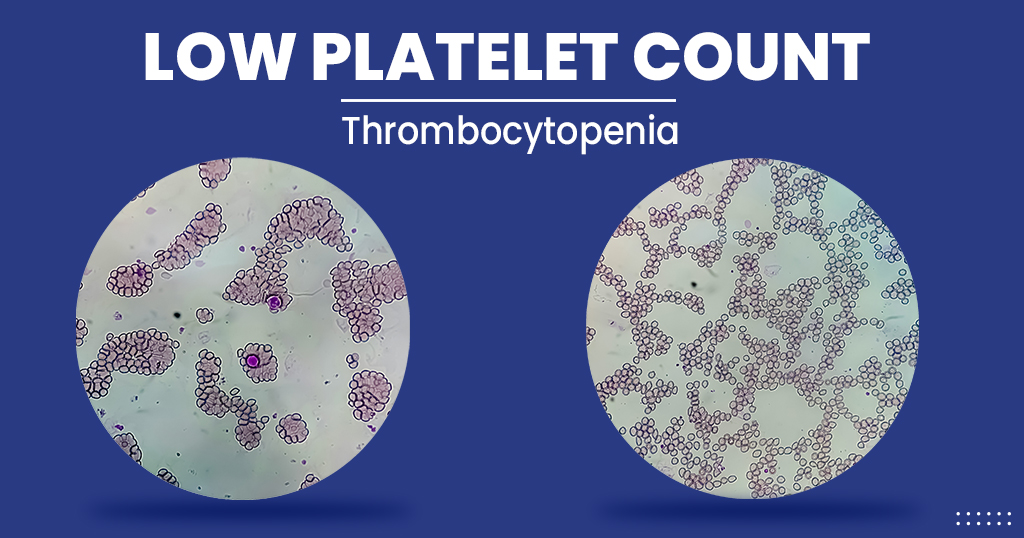
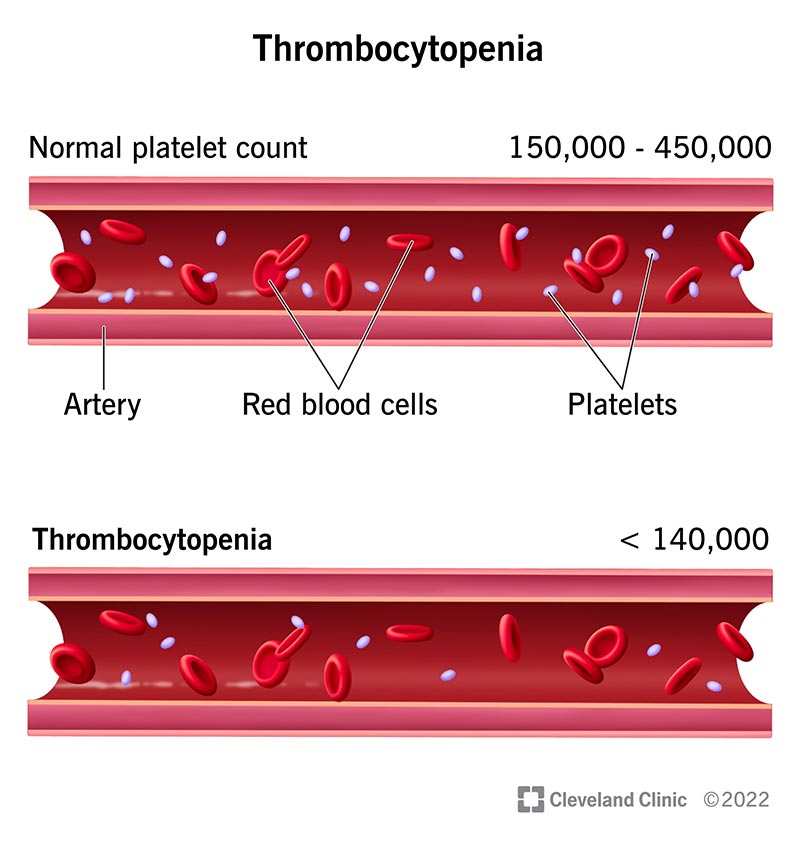
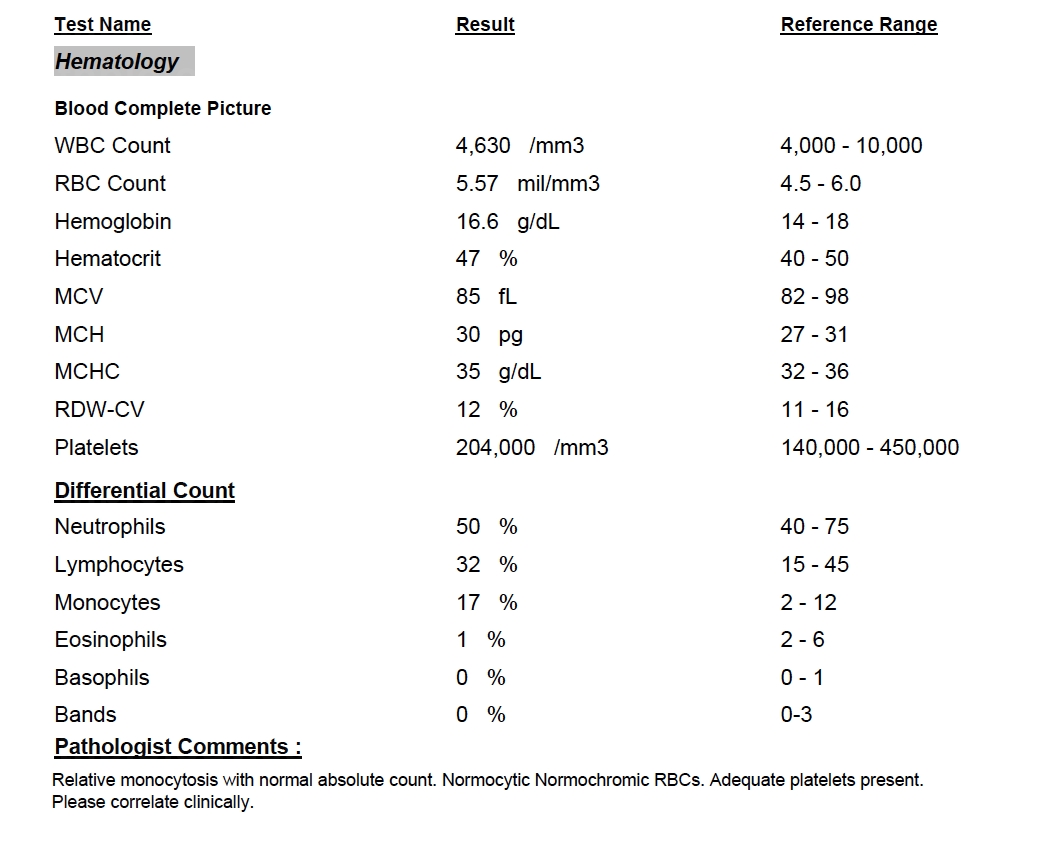
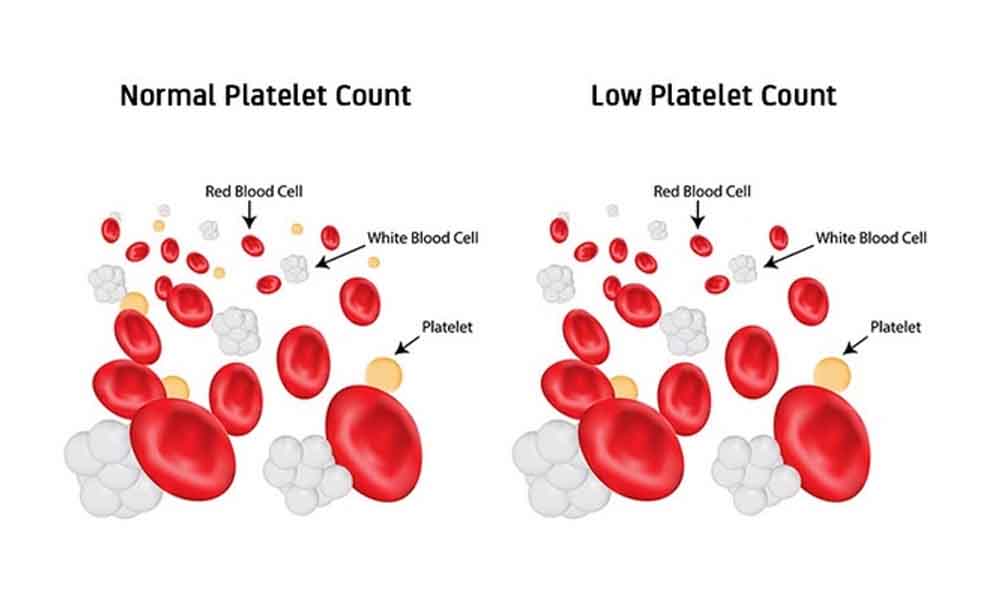
Aim to investigate cancer incidence following a normal platelet count in primary care.1 a normal platelet count falls between 150 and 450 × 10 9 /l and varies with the age and sex of the individual.Volume of distribution at steady state in healthy subjects was estimated to be 275 l (17%).
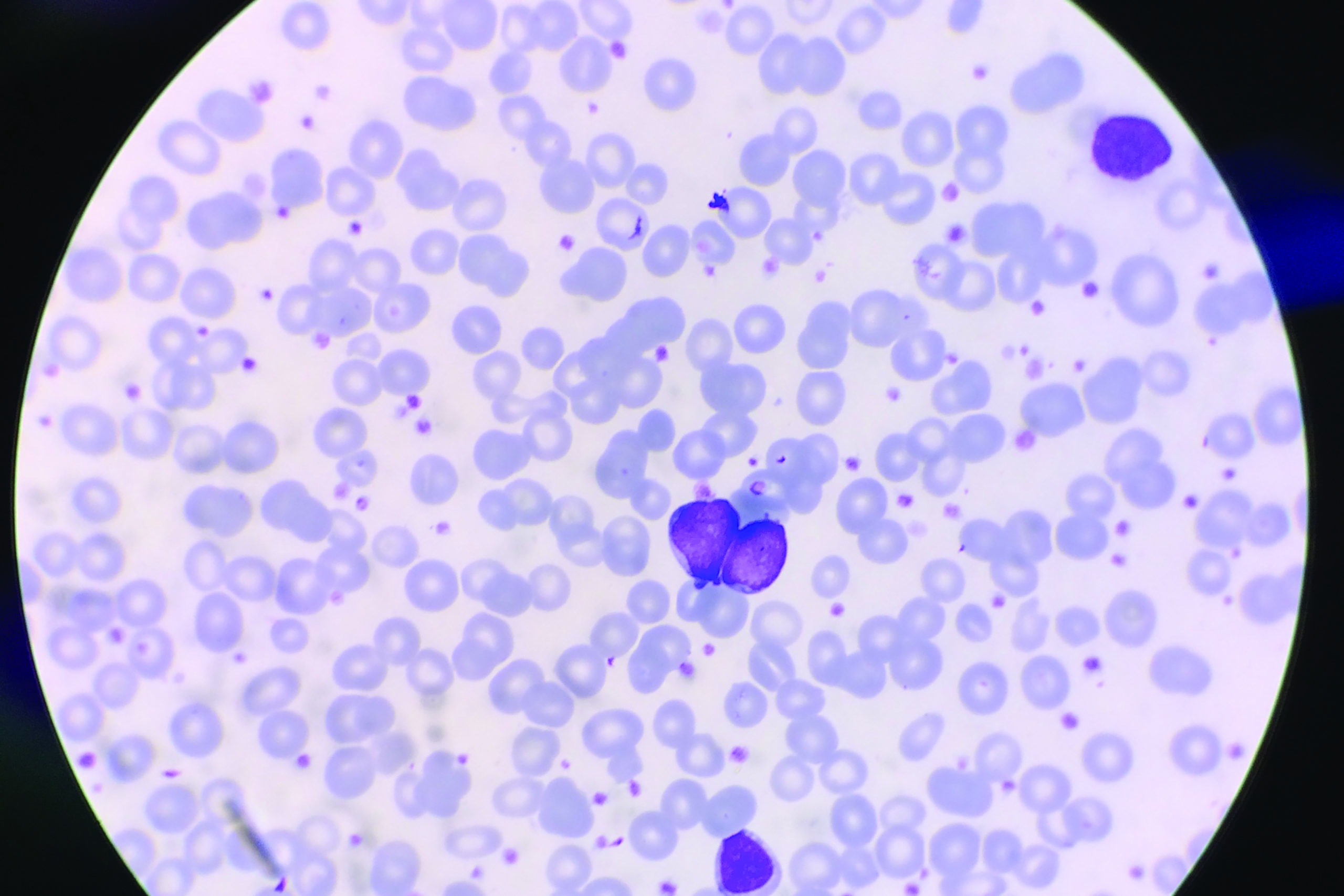
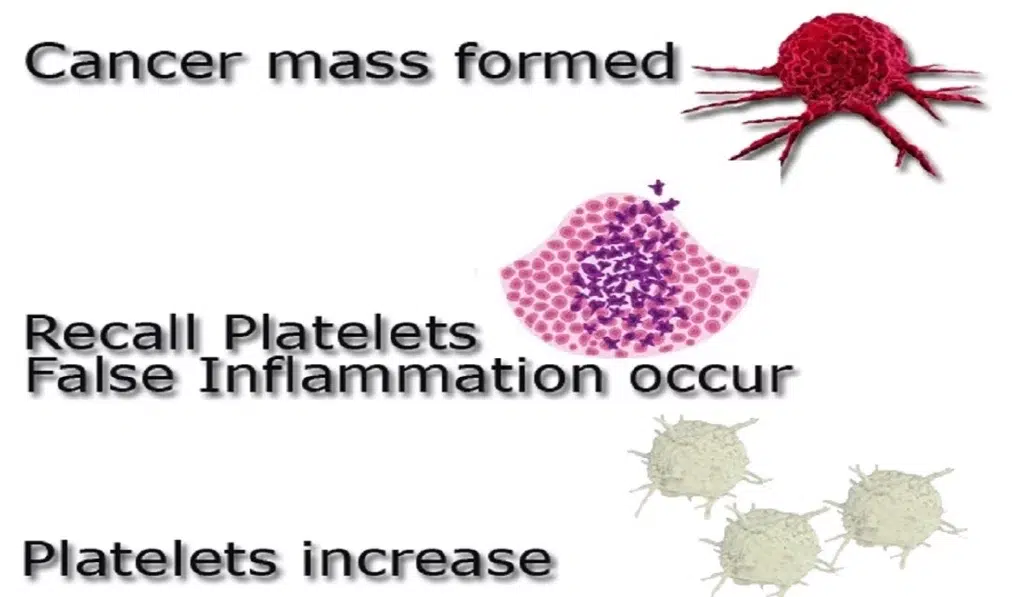
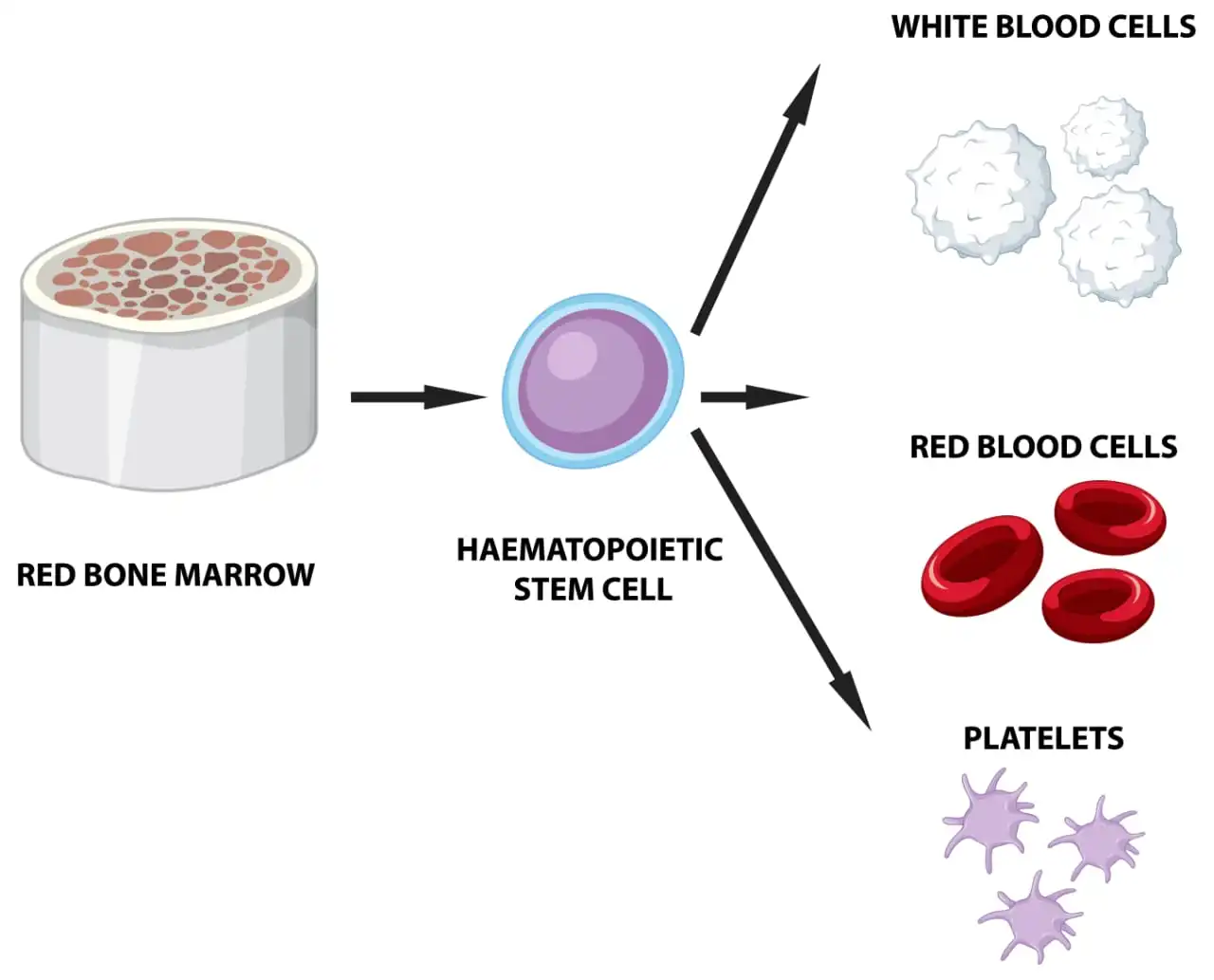
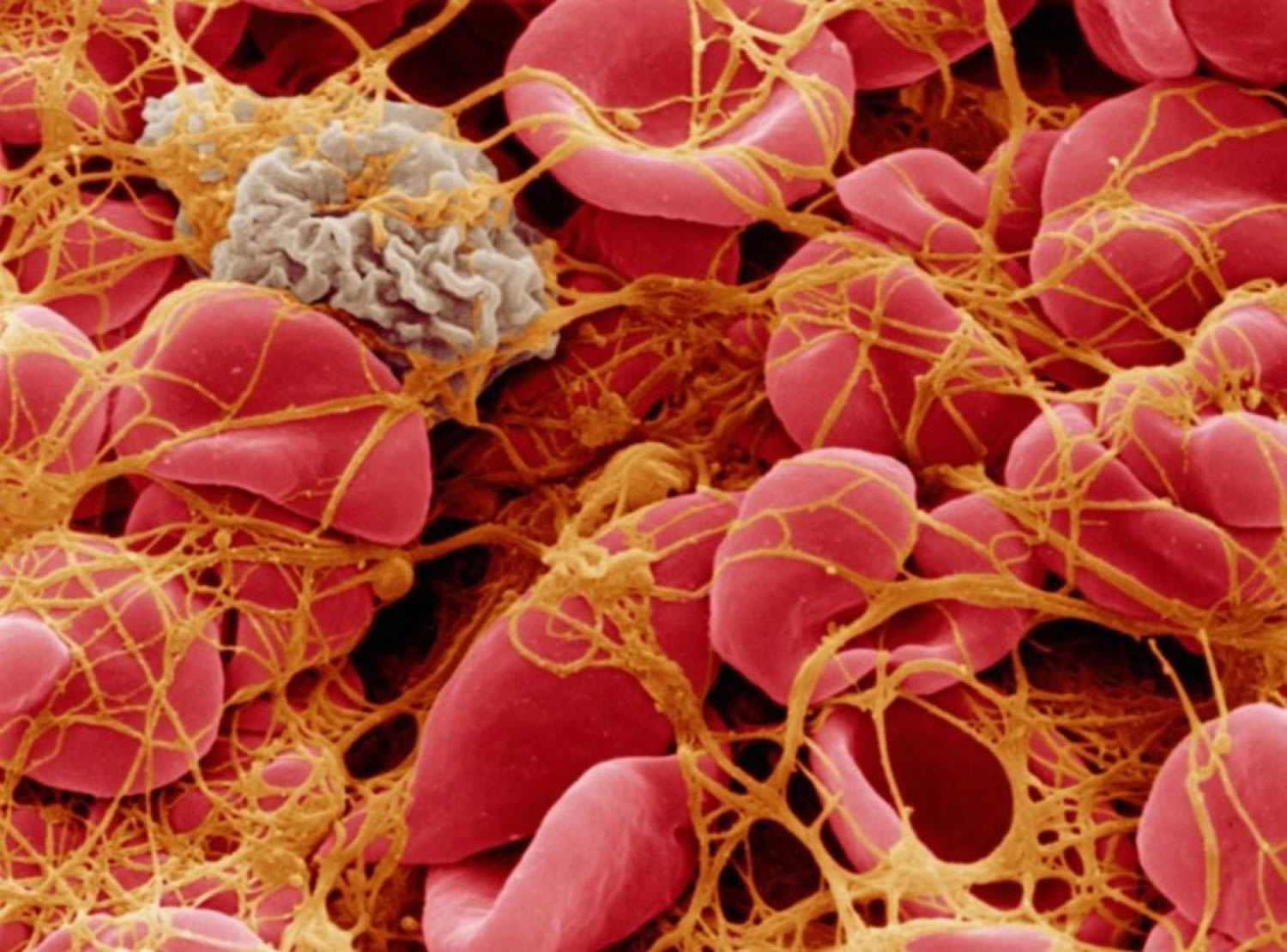
In this review, we present a detailed picture of the dynamic roles of platelets in tumour development and progression as well as their use in diagnosis, prognosis and monitoring response to therapy.Platelets, the smallest proteins that make up blood, are responsible for causing clots at the site of injury to prevent further blood loss.
Another reason for secondary thrombocytosis is when the spleen has been removed.Normalization of nlr in patients with baseline elevation was associated with longer median os and response to therapy.However, until recently, targeting platelets as a cancer therapeutic has been hampered by the elevated risk of haemorrhagic and thrombocytopenic (low platelet count) complications owing to the.
Thrombocytosis is generally defined as a raised platelet count >450x10 9 /l.43.8 months, p =.003), and nlr ≥ 3 (17.5 months.
Also, there is accumulating evidence that thrombocytosis (i.e., a platelet count above 400 × 10 9 platelets/l) is an independent predictor of poor prognosis in various types of cancer.However, the value of platelet count as a.
Last update images today Cancer With High Platelet Count
 Man United Extend Ten Hag Deal Through 2026
Man United Extend Ten Hag Deal Through 2026
The uncertainty around the future of Pakistan white-ball captain Babar Azam as well as the fate of the selection committee lingers as head coach Gary Kirsten and selector Wahab Riaz submitted their tour reports to PCB chairman Mohsin Naqvi following Pakistan's disappointing T20 World Cup campaign. Pakistan were dumped out of the tournament after just three games, with defeats to the USA and India proving terminal to their campaign.
The end of Pakistan's World Cup was followed by a fierce - and a somewhat frenzied - backlash in the country. The selection committee of seven, widely viewed as being de facto headed by Wahab, was one of its central targets, while a perceived tactical ineptitude and culture of conservatism under the captaincy of Babar has also come under scrutiny. There remain unanswered questions about the selection of the squad itself, particularly around the continued non-selection of specialist legspinner Abrar Ahmed despite Shadab Khan's indifferent form.
However, as ESPNcricinfo reported last month, the PCB has chosen to take its time before launching into any major decisions. Pakistan do not have a white-ball engagement until November, allowing the PCB to wait till Kirsten and Wahab - who was also the senior team manager for the tournament - handed in their reports.
It is understood the PCB remains open to a change of captaincy, though sticking with Babar has also not been conclusively ruled out. This partly stems from a lack of obvious candidates to replace him; when Naqvi decided to sack Shaheen Shah Afridi, he ultimately returned to Babar - who had only been replaced a few weeks earlier. That was following yet another poor showing at an ICC event - the ODI World Cup in India in 2023.
Now that Kirsten and Wahab have submitted their reports, any decisions regarding the "surgery" Naqvi had reportedly been prepared to conduct do theoretically move closer. However, the PCB has consistently refused to put a timeline on any action, insisting they wish to make a considered decision rather than a quick one.














:max_bytes(150000):strip_icc()/when-to-worry-about-high-platelet-count-5186732-Final-b4e4397cd12a47519b40e7388912542f.jpg)



:max_bytes(150000):strip_icc()/VWH-Michela-Buttignol-High-Platelet-Count-Standard-fee002ace1e34215801aa1ec08b82e4e.jpg)